WHEN IS THE BEST MOMENT TO APPLY PHOTOBIOMODULATION THERAPY (PBMT) WHEN ASSOCIATED TO A TREATMILL ENDURANCE-TRAINING PROGRAM? A RANDOMIZED, TRIPLE-BLINDED, PLACEBO-CONTROLLED CLINICAL TRIAL.
- By rgpodadmin
- November 16, 2023
ABSTRACT
Photobiomodulation therapy (PBMT) employing low-level laser therapy (LLLT) and/or light emitting diode therapy (LEDT) has emerged as an electrophysical intervention that could be associated with aerobic training to enhance beneficial effects of aerobic exercise. However, the best moment to perform irradiation with PBMT in aerobic training has not been elucidated. The aim of this study was to assess the effects of PBMT applied before and/or after each training session and to evaluate outcomes of the endurance-training program associated with PBMT. Seventy-seven healthy volunteers completed the treadmill-training protocol performed for 12 weeks, with 3 sessions per week. PBMT was performed before and/or after each training session (17 sites on each lower limb, using a cluster of 12 diodes: 4 × 905 nm super-pulsed laser diodes, 4 × 875 nm infrared LEDs, and 4 × 640 nm red LEDs, dose of 30 J per site). Volunteers were randomized in four groups according to the treatment they would receive before and after each training session: PBMT before + PBMT after, PBMT before + placebo after, placebo before + PBMT after, and placebo before + placebo after. Assessments were performed before the start of the protocol and after 4, 8, and 12 weeks of training. Primary outcome was time until exhaustion; secondary outcome measures were oxygen uptake and body fat. PBMT applied before and after aerobic exercise training sessions (PBMT before + PBMT after group) significantly increased (p < 0.05) the percentage of change of time until exhaustion and oxygen uptake compared to the group treated with placebo before and after aerobic exercise training sessions (placebo before + placebo after group) at 4th, 8th, and 12th week. PBMT applied before and after aerobic exercise training sessions (PBMT before + PBMT after group) also significantly improved (p < 0.05) the percentage of change of body fat compared to the group treated with placebo before and after aerobic exercise training sessions (placebo before + placebo after group) at 8th and 12th week. PBMT applied before and after sessions of aerobic training during 12 weeks can increase the time-to-exhaustion and oxygen uptake and also decrease the body fat in healthy volunteers when compared to placebo irradiation before and after exercise sessions. Our outcomes show that PBMT applied before and after endurance-training exercise sessions lead to improvement of endurance three times faster than exercise only.
INTRODUCTION
Physical activity is recommended and beneficial for both asymptomatic persons and individuals with chronic diseases [1, 2]. Aerobic endurance is considered a useful tool for the assessment of physical fitness and the detection of changes in aerobic fitness resulting from systematic training [3].
Regular aerobic exercise has various beneficial metabolic, vascular, and cardiorespiratory effects [4]. Additionally, it decreases body fat and increases muscle mass, muscle strength, and bone density [5]. Moreover, it improves self-esteem and physical and mental health and reduces the incidence of anxiety and depression [4, 6].
Various ergogenic agents, such as whey protein [7], caffeine [8], creatine [9], and neuromuscular electrical stimulation [10], are currently used to increase the benefits of aerobic training. Photobiomodulation therapy (PBMT) has emerged as an electrophysical intervention that could be associated with aerobic training to enhance beneficial effects of aerobic exercise, since several studies used PBMT to improve physical performance when associated with different kinds of exercise [11, 12, 13, 14].
Several studies have recently used PBMT to improve muscle performance during aerobic activities in healthy adults [15, 16, 17, 18] and postmenopausal women [19, 20]. However, to the best of our knowledge, the best moment to perform irradiation with PBMT in aerobic training has not been yet elucidated.
For instance, the current literature shows that the application of PBMT before progressive aerobic exercise has ergogenic effects and acutely increases the time until exhaustion, covered distance, and pulmonary ventilation and decreases the score of dyspnea during progressive cardiopulmonary test [15]. In addition, PBMT irradiation performed prior to aerobic exercises improves the exercise performance by decreasing the exercise-induced oxidative stress and muscle damage [18] and increasing the oxygen extraction by peripheral muscles [16]. When performed during aerobic training sessions, PBMT improves the quadriceps power and reduces the peripheral fatigue in postmenopausal women [19, 20]. Additionally, when applied after the sessions of endurance-training program, PBMT leads to a greater fatigue reduction than endurance training without PBMT irradiation [17].
Therefore, the optimal moment to perform PBMT in aerobic training is still open to discussion. With this perspective in mind, we aimed to assess the effects of PBMT applied at different time points (before and/or after) of each training session and its potential effects on the outcomes of an endurance-training program (aerobic exercise).
MATERIALS AND METHODS
STUDY DESIGN AND PROTOCOL
We performed a triple-blind (assessors, therapists, and volunteers), placebo-controlled, randomized clinical trial. The study was conducted in the Laboratory of Phototherapy in Sports and Exercise.
ETHICAL ASPECTS
All participants signed informed consent prior to enrollment and the study was approved by the research ethics committee of Nove de Julho University (process 553.831) and registered at Clinical Trials.gov (NCT02874976).
SAMPLE
The sample size was calculated assuming a type I error of 0.05 and a type II error of 0.2, based on previous study [21], and the primary established outcome was the time until exhaustion.
INCLUSION AND EXCLUSION CRITERIA
We recruited 96 healthy volunteers (48 men and 48 women) between 18 and 35 years of age and without training or involvement in a regular exercise program (i.e., exercise more than once per week) [22, 23]. Volunteers were excluded if they had any skeletal muscle injury, used any nutritional supplement or pharmacologic agent, presented with signs or symptoms of any disease (i.e., neurologic, inflammatory, pulmonary, metabolic, oncologic), or had a history of cardiac arrest that might limit performance of high-intensity exercises. Volunteers that were unable to attend a minimum rate of 80% of the training sessions and volunteers with immune diseases that require continuous use of anti-inflammatory drugs were also excluded.
RANDOMIZATION AND BLINDING PROCEDURES
Volunteers were distributed in four experimental groups (24 volunteers in each group) through a simple drawing of lots (A, B, C, or D) that determined the moment they would receive active and/or placebo PBMT treatment:
PBMT + PBMT: volunteers were treated with active PBMT before and after each training session.
PBMT + placebo: volunteers were treated with active PBMT before and placebo PBMT after each training session.
Placebo + PBMT: volunteers were treated with placebo PBMT before and active PBMT after each training session.
Placebo + placebo: volunteers were treated with placebo PBMT before and after each training session.
Randomization labels were created by using a randomization table at a central office where a series of sealed, opaque, and numbered envelopes ensured confidentiality. The researcher who programmed the PBMT device (manufactured by Multi Radiance Medical™, Solon, OH, USA) based on the randomization results was not involved in any other procedure of the study. He was instructed not to inform the participants or other researchers of the PBMT program (active or placebo). None of the researchers involved in aerobic endurance-training assessments and data collection knew which program corresponded to active or placebo PBMT.
Identical PBMT devices were used in both programs (active or placebo) by a researcher who was not involved in any phase of the projected data collection to ensure the study blinding. All displays and sounds emitted were identical regardless of the selected program. The active PBMT treatment did not demonstrate discernable amounts of heat [24].
Therefore, volunteers were unable to differentiate between active or placebo treatments. All volunteers were required to wear opaque goggles during treatments to safety and to maintain the triple-blind design.
PROCEDURES
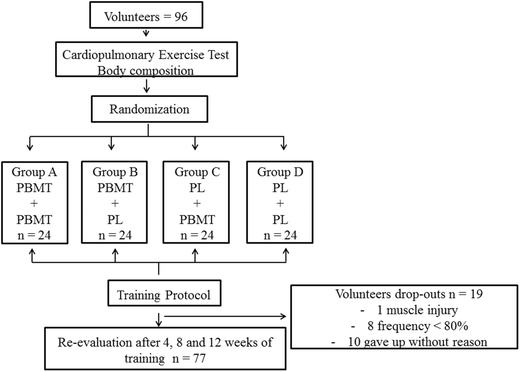
The study included three sessions of aerobic endurance training per week performed over 12 weeks, and each session lasted 30 min; the load for each exercise session (treadmill speed) progressed constantly in order to keep subjects’ heart rate between 70 and 80% from maximum heart rate. The assessments were conducted before the start of the training protocol and after 4, 8, and 12 weeks of training. A summary of the study design is presented in Fig. 1.
Open image in new window
Fig. 1
CONSORT flowchart
CARDIOPULMONARY EXERCISE TEST
Participants performed a standardized progressive cardiopulmonary exercise test on a treadmill with a fixed inclination of 1% until exhaustion. They began the test with a 3-min warm-up at a velocity of 3 km/h. Next, the treadmill velocity was increased by 1 km/h at 1-min intervals until the velocity of 16 km/h was reached. Participants were instructed to use hand signals to request termination of the test at any time. A 3-min recovery phase at a velocity of 6 km/h was allowed after each test [18]. During testing, we monitored the rates of oxygen uptake (VO2), carbon dioxide production measured with a VO 2000 gas analyzer (Inbrasport, Indústria Brasileira de Equipamentos Médico-Desportivos LTDA, Porto Alegre, RS, Brazil), total time until exhaustion, and heart rate measured with a digital electrocardiograph (Medical Graphs Ergomet, São Paulo, SP, Brazil).
These data were used to evaluate the performance of participants during progressive cardiopulmonary exercise testing, because this test is currently the most widely used in the literature for this purpose [25]. The entire test was monitored by electrocardiogram and blood pressure measurement. If any abnormal heart rate or blood pressure changes were observed or if the test was terminated prematurely on request, the test was stopped, and the volunteer’s data were deleted.
BODY COMPOSITION ASSESSMENT
Body composition was assessed by the same technician (blinded to volunteer’s allocation in different experimental groups) using the procedures established by ISAK [26]. Measurements of height, body mass, and skinfolds were used to establish the percentage of fat [26].
AEROBIC TRAINING PROTOCOL
Aerobic treadmill training, associated or not with PBMT, was performed three times a week for 12 weeks, each session lasting 30 min, with training intensity kept between 70 and 80% of maximum heart rate [27]; changes in running speed (training load) were constantly performed to achieve the 70–80% heart rate.
Training was interrupted based on the criteria established by the guidelines of the American Heart Association. Training intensity was monitored by a heart rate monitor manufactured by Polar®.
PHOTOBIOMODULATION THERAPY
PBMT was applied employing MR4 Laser Therapy Systems outfitted with LaserShower 50 4D emitters (both manufactured by Multi Radiance Medical, Solon, OH, USA). The cluster style emitter contains 12 diodes composing of four super-pulsed laser diodes (905 nm, 0.3125 mW average power, and 12.5 W peak power for each diode), four red LED diodes (640 nm, 15 mW average power for each diode), and four infrared LEDs diodes (875 nm, 17.5 mW average power for each diode).
The cluster probe was selected due to the available coverage area and to reduce the number of sites needing treatment. Treatment was applied in direct contact with the skin with a slight applied overpressure to nine sites on extensor muscles of the knee (Fig. 2a), six sites on knee flexors of the knee, and two sites on the calf (Fig. 2b) of both lower limbs [15, 28]. To ensure blinding, the device emitted the same sounds and regardless of the programmed mode (active or placebo). The researcher, who was blinded to randomization and the programming of PBMT device, performed the PBMT.
Open image in new window
Fig. 2
a Treatment sites at knee extensor muscles. b Treatment sites at knee flexor and ankle plantar flexor muscles
PBMT parameters and irradiation sites were selected based upon previous positive outcomes demonstrated with the same family of device [13, 15, 28, 29]. Table 1 provides a full description of the PBMT parameters. The volunteers received PBMT or placebo from 5 to 10 min before and/or after aerobic training sessions.
STATISTICAL ANALYSIS
The obtained results were tested for their normality through the Shapiro-Wilk test. Since the data showed a normal distribution, two-way ANOVA test with Bonferroni post hoc analysis was applied. The data were described as mean values with the respective standard deviations and both absolute and percentage values were analyzed. Graphical data are described as mean and standard errors of mean (SEM). The level of statistical significance was p < 0.05. RESULTS After data collection, we analyzed the results of 77 volunteers of both genders (PBMT + PBMT: 18 volunteers; PBMT + placebo: 21 volunteers; placebo + PBMT: 18 volunteers; and placebo + placebo: 20 volunteers) that had completed the aerobic training protocol after 12 weeks (Fig. 1). None of the recruited volunteers were excluded due abnormal heart rate or blood pressure during the execution of procedures of this study. The characteristics of the volunteers are summarized in Table 2. As shown in Table 2, no statistically significant differences (p > 0.05) were found for anthropometric variables and baseline data among the different experimental study groups.
Table 3 shows all results of cardiopulmonary progressive test in absolute values for different variables analyzed in all experimental groups of this study. We observed a statistically significant improvement in oxygen uptake when PBMT was performed before and after training sessions (PBMT + PBMT group), comparing baseline values vs 4-, 8-, and 12-week values (p < 0.001). The same was observed for pulmonary ventilation, comparing baseline values vs 8- and 12-week values (p = 0.0018 and p = 0.003, respectively), and for time until exhaustion, comparing baseline values vs 4-, 8-, and 12-week values (p < 0.001).
Table 3
Progressive endurance test variables
Baseline
4 weeks
8 weeks
12 weeks
VO2 (mL/kg/min)
PBMT + PBMT
35.8 ± 9.5
40.2 ± 10.2*
41.5 ± 10.4*
42.5 ± 11.2*
PBMT + Placebo
34.8 ± 7.0
37.6 ± 7.0
38.6 ± 8.0
38.2 ± 7.0
Placebo + PBMT
35.2 ± 8.9
36.6 ± 8.1
38.6 ± 8.3
38.5 ± 8.3
Placebo + placebo
36.2 ± 7.7
36.8 ± 8.0
37.6 ± 7.5
38.4 ± 10.1
VCO2 (mL/kg/min)
PBMT + PBMT
38.7 ± 7.0
40.4 ± 8.6
41.3 ± 7.8
41.4 ± 8.7
PBMT + placebo
38.,5 ± 7.8
39.5 ± 6.6
41.7 ± 7.9
41.9 ± 6.8
Placebo + PBMT
38.5 ± 9.5
38.2 ± 9.5
41.5 ± 8.4
40.7 ± 9.6
Placebo + placebo
38.8 ± 10.6
40.7 ± 9.4
43.1 ± 13.4
40.9 ± 10.5
VE (mL/kg/min)
PBMT + PBMT
73.6 ± 22.8
77.9 ± 21.5
83.5 ± 24.5*
85.3 ± 22.5*
PBMT + Placebo
70.6 ± 20.3
71.0 ± 23.1
78.1 ± 23.0
77.2 ± 22.1
Placebo + PBMT
66.2 ± 25.3
70.6 ± 24.2
73.9 ± 20.6
73.4 ± 20.7
Placebo + placebo
69.9 ± 17.9
70.8 ± 18.8
70.3 ± 22.4
77.1 ± 18.3
Time until exhaustion (s)
PBMT + PBMT
681.5 ± 111.9
752.1 ± 111.7*
787.7 ± 114.2*
808.5 ± 124.5*
PBMT + placebo
698.7 ± 131.1
739.3 ± 142.2
773.4 ± 165.9
792.1 ± 186.9
Placebo + PBMT
693.1 ± 106.9
738.4 ± 116.6
766.1 ± 121.0
797.0 ± 139.0
Placebo + placebo
699.5 ± 137.3
720.2 ± 150.0
741.3 ± 154.3*
766.1 ± 159.8*
Data is expressed in average and standard deviation (±)
VO 2 oxygen uptake, VCO 2 carbon dioxide production, VE pulmonary ventilation
*Statistically significant difference compared to baseline (p < 0.05)
Furthermore, PBMT applied before and after each aerobic exercise training session (PBMT + PBMT group) significantly increased (p < 0.05) the percentage change of oxygen consumption and time-to-exhaustion compared to the group treated with placebo before and after each aerobic exercise training session (placebo + placebo group) from 4th to 12th week. Similarly, PBMT applied before and after each aerobic exercise training session (PBMT + PBMT group) significantly improved (p < 0.05) the percentage change of body fat compared to group treated with placebo before and after each aerobic exercise training session (placebo + placebo group). The outcomes are summarized in Figs. 3, 4, and 5, respectively.
Open image in new window
Fig. 3
Percentage of change in time-to-exhaustion. The data are presented in mean and SEM. Letter a indicates statistical significance between PBMT + PBMT and placebo + placebo (p < 0.05)
Open image in new window
Fig. 4
Percentage of change in maximum oxygen uptake. The data are presented in mean and SEM. Letter a indicates statistical significance between PBMT + PBMT and placebo + placebo (p < 0.05)
Open image in new window
Fig. 5
Percentage of change in body fat. The data are presented in mean and SEM. Letter a indicates statistical significance between PBMT + PBMT and placebo + placebo (p < 0.05)
DISCUSSION
To the best of our knowledge, this is the first study aiming to test the optimal moment to perform PBMT in an aerobic training protocol (before, after, or before and after training). Few studies have assessed chronic effects of PBMT [17, 20, 21]; however, PBMT has been applied at different moments (before, after, or during exercise) of the aerobic training program. Briefly, we observed that the combination of super-pulsed lasers and LEDs applied before and after exercise sessions increased the oxygen uptake, time-to-exhaustion, and reduced body fat in healthy sedentary volunteers after 12 weeks of aerobic training.
Paolillo et al. [20] investigated the effects of PBMT applied during the sessions of aerobic training on the treadmill in 20 postmenopausal women. The training was performed twice a week for 3 months, with an intensity of 85–90% of maximum heart rate. The volunteers received LED therapy with 850 nm, 31 mW/cm2, 30 min irradiation, and 14,400 J applied bilaterally to the tight regions. PBMT increased the exercise tolerance time when compared to the control group. These data corroborate with the results of our study, however, we used different light sources and wavelengths simultaneously (4 × 905 nm super-pulsed lasers, 4 × 875 nm infrared LEDs, and 4 × 640 nm red LEDs) to irradiate the volunteers and we found an increase in exercise tolerance of 13.4%. The magnitude of the difference in outcomes between studies might be related to the used irradiation protocol (in our study, the volunteers were irradiated before and after the aerobic training sessions, while Paolillo et al. [20] irradiated volunteers during the training sessions).
The same authors [21] also investigated the effects of PBMT (infrared LEDs—850 nm) when applied during treadmill training in 45 postmenopausal women. The training was performed twice a week for 6 months, and each training session lasted 45 min. The authors found a significant increase in exercise tolerance, and metabolic equivalents, and a longer duration of Bruce test. In our study, the association of PBMT before and after sessions of the aerobic training program was able to increase the oxygen consumption (with 18.7%) and time-to-exhaustion (with 13.4%) and improve the percentage of change of body fat (with 13.9%) after only 12 weeks of aerobic training.
Duarte et al. [30] evaluated the effects of PBMT (808 nm) associated with aerobic and resistance training performed three times a week for 16 weeks in obese women. The authors found a significant decrease in the percentage of fat and in neck and waist circumference. It is important to highlight that in our study, we observed statistically significant improvement in the percentage of change of body fat (13.9%) after only 12 weeks of aerobic training when associated with PBMT before and after the training sessions. We believe that the association of PBMT before and after training was able to enhance the performance and the tolerance of the volunteers during the aerobic training protocol, favoring the reduction of the body fat at the end of the 12 weeks of training.
It is interesting how outcomes in the fourth week for PBMT + PBMT group were similar to those of placebo + placebo group (or exercise alone) in the 12th week. This means that PBMT with optimal irradiation protocol (before and after exercise training sessions) can increase the endurance capacity of volunteers three times faster than exercise alone.
Regarding the mechanisms of the observed effects, we strongly believe that mitochondrial activity modulation is the key mechanism, despite the fact that our study only focused on clinical and functional aspects and not on mechanisms. Hayworth et al. [31] demonstrated that the activity of cytochrome c oxidase is enhanced by PBMT with a single wavelength in skeletal muscle fibers of rats. More recently, Albuquerque-Pontes et al. [32] showed that PBMT with different wavelengths (660, 830, or 905 nm) was able to increase the expression of cytochrome c oxidase in the intact skeletal muscle tissue in different time windows (5 min to 24 h after irradiation), which means that the muscle metabolism can be improved through the action of PBMT. These findings help us to explain the increase in performance observed by the use of PBMT associated with an aerobic training protocol and provide the rationale for the concurrent use of different wavelengths at the same time, which can represent a therapeutic advantage in various clinical situations.
In fact, different studies have shown that the concurrent use of different light sources and wavelengths enhances muscular performance [13, 14, 15, 28, 29, 33] decreases pain [34
Original Source: https://link-springer-com.colorado.idm.oclc.org/article/10.1007%2Fs10103-017-2396-2